To the new parents who are awaiting the arrival of, or are already cherishing time with, your beloved baby—I offer my warmest congratulations and support. This period, however, often brings moments of joy mixed with anxiety and difficult emotions. You may find terms like ‘prenatal depression’ or ‘postpartum depression’ unfamiliar, or think, “That won’t happen to me.”
As a fellow parent who has walked this path, I want to share honest and detailed insights into the “common but often overlooked cold of the mind”—prenatal and postpartum depression—that can occur during the major transition of pregnancy and childbirth. This is not something to hide or suffer through alone; it is a mental health concern that requires attention. I hope this article empowers you to care for yourself, understand each other, and begin your parenting journey in a healthy way.

1. What Are Prenatal and Postpartum Depression?
| Category | Typical Onset Period | Key Characteristics |
| Prenatal (Antenatal) Depression | Anytime during pregnancy | Persistent feelings of sadness, lethargy, anxiety, and insomnia during pregnancy. Often accompanied by vague fears about childbirth or the pressure of the mothering role. |
| Postpartum Depression (PPD) | Within 4 weeks after delivery (can last up to a year) | Symptoms are more severe and last longer than 2 weeks compared to the general ‘Baby Blues.’ It is a depressive disorder that interferes with daily life and the ability to care for the baby. |
| Postpartum Blues (Baby Blues) | Starts 2-4 days post-delivery, resolves within 2 weeks | Temporary mood swings, tearfulness, irritability, and anxiety. Considered a normal experience, affecting up to 85% of new mothers. |
2. Why Does It Occur? (Causes)
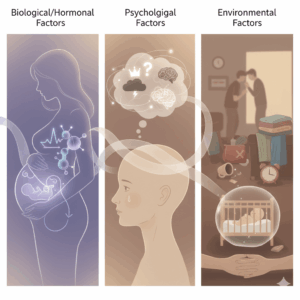
Perinatal depression stems from a complex interplay of factors, not a single cause.
- Sudden Hormonal Changes: The sharp drop in female hormones (estrogen, progesterone) after childbirth is the primary biological trigger. (During pregnancy, hormonal shifts and physical discomfort are key factors).
- Psychological Factors: The overwhelming pressure of the new role as a mother (or father), the compulsion to be a ‘perfect’ parent, and the stress and fear surrounding childbirth and childcare.
- Environmental Factors: Chronic fatigue and lack of sleep, physical pain from delivery, insufficient social support (from partner, family), marital conflict, and financial strain.
- Previous History: A higher risk exists for those with a prior history of mental health issues like depression, anxiety disorders, or severe Premenstrual Syndrome (PMS).
3. How Does It Differ from General Depression?
Perinatal depression includes all the common symptoms of Major Depressive Disorder (sadness, loss of interest, changes in sleep/appetite) but also features unique symptoms related to pregnancy/childbirth and the relationship with the baby.
- Problems with Bonding: Experiencing excessive worry about the baby, or conversely, lack of interest or concern for the baby, feeling guilty or struggling with childcare.
- Intrusive Thoughts (Obsessions): Experiencing intrusive thoughts or impulses about harming oneself or the baby (infanticide). This is a severe symptom requiring immediate professional help.
4. How is it Treated, and Can it Resolve Naturally?
While mild Postpartum Blues often resolve naturally within two weeks, Prenatal and Postpartum Depression that lasts longer than two weeks is a ‘treatable illness’ that requires intervention.
- Natural Recovery: Symptoms can persist for over a year without treatment, and there is a high risk of worsening or recurrence if left untreated. Do not wait for it to resolve on its own.
- Main Treatment Methods:
- Psychotherapy (Talk Therapy): Cognitive Behavioral Therapy (CBT), Interpersonal Therapy (IPT), couples therapy, and therapies focused on improving mother-infant interaction are recommended.
- Medication: For moderate to severe depression, or when psychotherapy alone is insufficient, a psychiatrist can prescribe antidepressants that are safe for breastfeeding after consultation. (Can also be taken during pregnancy after consulting a specialist.)
- Supportive Care: Ensuring adequate rest and sleep, maintaining a regular lifestyle, and receiving proactive support and help from the partner and family.

5. Self-Diagnosis: Checking Your Symptoms
If you experience 5 or more of the following symptoms most days for two weeks or more, it is advisable to seek professional advice:
- Feeling depressed or sad most of the day.
- Loss of interest or pleasure in activities you once enjoyed.
- Significant change in appetite (decrease or increase) or weight.
- Sleep disturbance (insomnia or sleeping excessively).
- Increased irritability, anxiety, or restlessness.
- Severe fatigue and loss of energy.
- Feelings of worthlessness or excessive guilt.
- Impaired concentration or memory.
- Marked lack of interest in the baby, or thoughts of harming the baby.
- Thoughts of self-harm or suicide. (Seek immediate help if this occurs.)
6. Supporting a Loved One: Recognizing Signs and Offering Help
The partner is the closest supporter and is often the first to notice signs of distress. The role of the husband/partner is paramount.
✅ Recognizing Warning Signs
- Frequent crying spells without clear reason, severe irritability, and extreme mood swings.
- Marked lack of interest in caring for the baby, or conversely, excessive worry.
- Significant changes in sleep patterns (severe insomnia or constant sleeping).
- Complaining that no one is looking after them, or attempting to socially isolate.
- Complaints of body discomfort or pain that have no apparent medical cause.
🤝 Practical Ways to Help
- Active Co-Parenting and Chore Sharing: Proactively help with tasks that relieve the mother’s burden, such as changing diapers, taking night feeding shifts, and doing housework.
- Emotional Support: Avoid blaming or criticizing her feelings. Instead, validate and reassure her by saying, “This is not your fault; it’s an illness, and we can treat it.”
- Avoid Criticism of Appearance: Refrain from making any negative comments, even as a joke, about weight or appearance changes after childbirth. Increase affection and positive affirmation.
- Ensure Adequate Rest: Create an environment where the mother can have time alone and get sufficient sleep. Lack of sleep is a major factor in worsening depression.
- Connect with a Professional: If symptoms persist for more than two weeks, actively encourage and accompany her to a mental health professional or a local community support center.
7. Does it Affect the Baby?
Yes, it can. If PPD persists, poor mother-infant interaction can negatively impact the baby’s emotional, social, and cognitive development. However, this is recoverable with treatment, and experts emphasize that the mother’s treatment is essential to minimize any negative effects on the child.
8. How to Prevent It?
While you can’t prevent it entirely, there are steps to reduce risk factors and alleviate symptoms.
- Gain Knowledge and Set Expectations: Learn about pregnancy, childbirth, and newborn care in advance to reduce vague fears.
- Healthy Lifestyle: Maintain physical health through proper nutrition and regular, moderate exercise during pregnancy.
- Prioritize Rest and Sleep: Post-delivery, it is critical to get as much rest and sleep as possible, even if it means sleeping when the baby sleeps.
- Communication and Conflict Resolution: Throughout the pregnancy, share your feelings with your partner and discuss parenting and chore-sharing plans to minimize conflict.
- Secure Support: Identify and establish a social support network (family, friends, community programs, healthcare providers) from whom you can seek help.

As a fellow parent, the final encouragement I want to give you is this:
“Admitting that you are struggling is not a sign of failure as a parent. It is, in fact, the most courageous and wisest action you can take to protect your family.”
Prenatal and postpartum depression are temporary difficulties that can affect anyone. It is not your fault, and it is not something to be overcome solely through willpower—it is an illness that requires professional help.
Partners, be your loved one’s strongest shield. When they are struggling, replace blame with warmth, and hold them close, saying, “You are a wonderful parent, and I am here for you.” Parenting is a shared mission, not a solo endeavor.
This period will eventually pass. Take a moment to pause, breathe, and give yourself the time to heal with professional support. Your happiness as parents is the foundation of your baby’s happiness.
You are not alone. We are all on this journey together, and there are people ready to help you. Stay strong!